Three years ago, a nationwide infant formula shortage shook America, and before long led to fights at grocery stores and stories like this flooding the media:
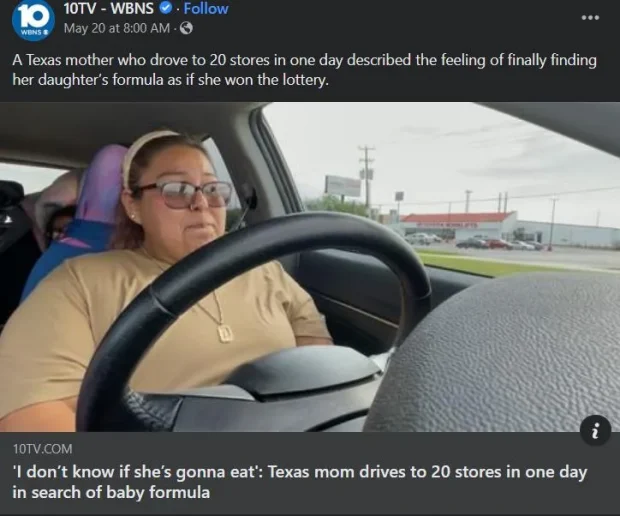
At the time, significant outrage was directed at the FDA since the shortage was due to pre-existing COVID-19 supply chain shortages exacerbated by a major recall by one of the leading formula producers (as at least two infants had recently died from contaminated formula, and the FDA had found the responsible bacteria at a major infant formula plant) which was then further exacerbated by a wave of panic buying that emptied many grocery stores.
This then led to many people pointing out it was ridiculous the FDA was willing to pull America’s formula supply over a relatively small production issue, but simultaneously was unwilling to do anything about the mRNA vaccines despite the fact the contamination in them and the deaths they were causing were orders of magnitude greater than anything which could possibly be attributed to the suspect infant formula lines.
As I watched this unfold, my thoughts were a bit different. Could there possibly be another way to feed your infants? Perhaps one that you could do at home that did not rely upon an unstable supply chain. I thus looked into how the homesteading and alternative health communities were addressing this dilemma and came across things like this:

I thus took the events of 2022 as a remarkable testament to just how effectively the formula industry had convinced mothers they needed to do anything besides breastfeed their children. At the same time however, I was hopeful these events would catalyze a public shift on this issue, so since then, I’ve gradually tried to put out the key points needed to understand what’s gone awry with infant formula and facilitate that change.
In turn, RFK Jr. recently announced an FDA initiative to make America’s infant formula healthy again (e.g., conducting a comprehensive review of its nutritional content, testing formula for heavy metals, and objectively assessing the health issues that arise from being formula fed). I believe that for “Operation Stork Speed” to succeed, it’s critical to understand the context of what’s happened with infant formula.
Note: in addition to heavy metals (and other harmful chemicals), infant formula has also repeatedly been found to be contaminated with aluminum, something which is quite problematic due to its adverse effects on the physiologic zeta potential (which the nervous system is very sensitive to disruptions of).
The History of Formula Feeding
While I strongly believe in the value of breastfeeding, throughout history and cultures, there are many references of mothers who could not sufficiently nourish their children with breastmilk who then sought out milk from other mothers or other supplemental sources of infant nutrition (which unfortunately were often not nutritionally adequate or contaminated with microorganisms).
Note: I believe that one of the primary causes of insufficient milk production from the mother was poor nutrition or malnutrition (something which was addressed in many early societies by having mothers eat specific diets).
This led to a variety of attempts to create a milk substitute that more accurately matched the safety and efficacy of human breastmilk (starting in 1865), a process which was revolutionized through the discovery of evaporated milk powder and its adaptation into infant formulas in the early 1900s. That was followed by various other attempts to produce more nutritionally adequate formulas.
As infant formulas improved in the 1920s, manufacturers began targeting physicians with their advertising. By 1929, the American Medical Association (AMA) established a committee to evaluate the safety and quality of formula compositions, leading many companies to seek the AMA’s “Seal of Acceptance,” bringing physicians closer to formula manufacturers. By the 1940s and 1950s, formula use became widely accepted as a safe alternative to breastmilk, and with the help of aggressive marketing and the inappropriate medicalization of childbirth, successfully displaced breastfeeding.
Note: the AMA’s seal of approval was created in 1905, and was designed to be a source of revenue to keep the struggling organization afloat (as it was given in return for advertising dollars rather than any assurance of safety—for instance the AMA widely promoted the benefits of smoking their sponsor’s cigarette brand). Sadly, once this funding allowed the AMA to begin establishing a foothold in the medical market, the organization then switched to blacklisting every competing therapy which would not sell out to the AMA (which is essentially why there are so many remarkable forgotten medical therapies exist from the early 1900s).
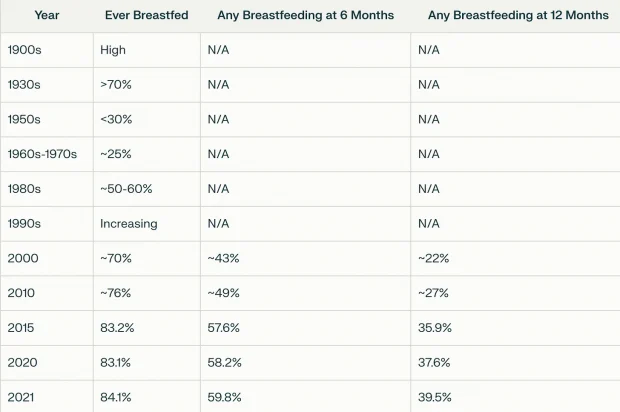
Many recognized this shift was harmful to both mothers and children. Hence, various groups (particularly the La Leche League, which was founded in 1956) mobilized the public to support breastfeeding mothers. In the 1970s, they finally reached the public (due to both scientific data emerging in support of breastfeeding and a growing societal dissatisfaction with the paternalistic and insensitive attitude medicine had to women). This shift began with middle-class mothers returning to natural breastfeeding, and gradually, governments eventually recognized the value of breastfeeding too (although it was not until 1984 that indecency laws against public breastfeeding began being updated). The decline in breastfeeding was, at last, reversed.
This chart combined a lot of different data sources.
One of the key events that catalyzed this shift away from formula was the Nestlé formula scandal (which began in 1973), which began after the public learned Nestlé was aggressively targeting poor women in undeveloped countries for infant formula sales. This was accomplish by paying hospitals to give free samples to mothers after delivery and telling mothers (frequently via sales reps impersonating nurses) that they would not be able to produce enough milk for their babies, which in turn let to the impoverished mothers frequently not only switching to infant formula but diluting it (as they could not afford standard doses). Millions of infants died as a result of these practices, and Nestlé eventually came under widespread public scrutiny (e.g., boycotts, celebrity protests, government investigations, and some of its predatory marketing practices being banned). The fact that Nestlé was able to convince millions of mothers to starve their babies to death again illustrates how predatory many of these marketing tactics were (particularly since some of those now outlawed practices still continue in the poorer nations).
Formula Marketing
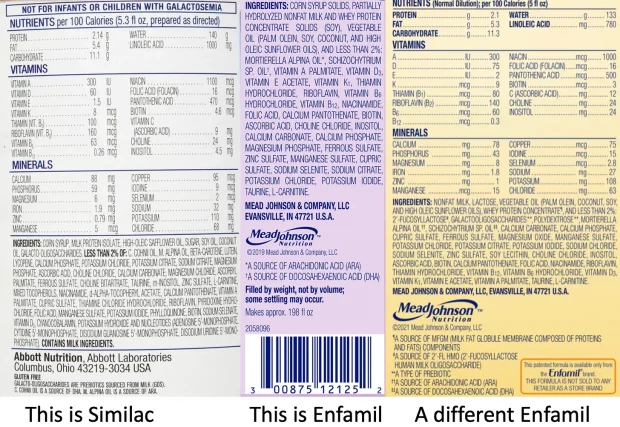
During each pediatric “well-child” visit, in addition to pushing the currently scheduled vaccines on the child, the child will also be weighed and often told that, according to the growth chart, they are underweight, strongly encouraged to consume infant formula, and sent home with a free sample. One of the particularly concerning things for me about doctors pushing these products on children was that the ingredients in the most common brands were fairly unhealthy:
Additionally, because of how frequently the “underweight” diagnosis came up, I naturally became quite suspicious of it.
Note: somewhat analogously, patients will routinely be told that due to their blood pressure and cholesterol, they are at a high risk of having a heart attack in the next few years, so they must start a statin to prevent it. Given that almost everyone ended up being “high risk,” I was not surprised to learn that in 2016, Kaiser completed an extensive study which determined this calculator overestimated the rate of these events by 600%. Sadly, that has not deterred doctors from using this calculator (e.g., medical students are still tested on it for their board examinations).
I then came across a passage from “How to Raise a Healthy Child In Spite of Your Doctor,” (written in 1987 by one of the original medical dissidents—Robert S. Mendelsohn) which stated the growth charts were extremely inaccurate (e.g., that they did not take into account a wide range of genetic variabilities in weight or that breast fed babies weighed less than formula fed ones) and that:
What their doctor doesn’t tell them is that this [weighing] ritual has no medical significance whatsoever. They aren’t told that some formula manufacturer was probably the source of the growth chart the doctor is using, and that he gets them free. That leads to an obvious question: Why are the formula makers so eager to have your doctor check your baby’s weight? Answer: Because the weight gain of breastfed babies may not match the average weights shown on the formula maker’s chart. They hope that the pediatrician, instead of reassuring the mother that this is normal and nonthreatening, will tell her to stop breastfeeding and switch to their product, of which he has a handy reminder in his hand. Too often, that si exactly what he does, and the baby is subsequently denied the immunity and other benefits that breastfeeding provides.
Given Mendelsohn’s accuracy, integrity, and knowledge as an insider, I was quite intrigued about this and discovered that during his career, many dubious weight charts had circulated around, and that it was not until 1977 that the US government made a standardized one. Following this, in 2000, the CDC made a chart using the average weights of American children (who were often on formula), and in 2006, the WHO made a chart using the weights of children who had been breastfed. The CDC chart (which is what’s often used in the United States) in turn, was recognized to be more prone to classify children as being underweight.
Below age 24 months, the revised [CDC] weight-for-age curves are generally higher than in the 1977 charts. This will result in more frequently classifying infants as underweight. Similarly, this shift would be expected to result in lower comparative estimates of overweight when the revised charts are used.
As expected, there are important differences between the WHO and CDC charts that vary by age group, growth indicator, and specific Z-score curve. Differences are particularly important during infancy, which is likely due to differences in study design and characteristics of the sample, such as type of feeding. Overall, the CDC charts reflect a heavier, and somewhat shorter, sample than the WHO sample. This results in lower rates of undernutrition (except during the first 6 mo of life) and higher rates of overweight and obesity when based on the WHO standards. Healthy breast-fed infants track along the WHO standard’s weight-for-age mean Z-score while appearing to falter on the CDC chart from 2 mo onwards.
Thus, the scam was:
•Infant formula is composed of ingredients that will make children overweight and obese (the first ingredient is often corn syrup and then followed by seed oils).
•Children who have been made overweight from the formula are the “new normal,” and anyone who weighs less than them is diagnosed as being underweight and pushed to take the formula (e.g., see this 2010 blog post by a pediatrician about it).
In turn, many studies (and systematic reviews) have found formula feeding not only causes rapid weight gain but also makes children much more likely to be obese as adults.1,2,3,4,5,6
As such, formula’s role in the continually increasing childhood obesity rates (e.g., 19.7% in 2020) must be considered (but unfortunately we are instead “solving” it by putting children on Ozempic—a drug which has a great deal of issues).
Later, I got in touch with one of the (now retired) doctors Mendelsohn mentored, who shared a few other important things with me:
Mendelsohn told me that during his appointment as Medical Director of Project Head Start’s Medical Consultation Service in 1968, he was horrified by the discussions held privately in the White House with his medical colleagues. They were openly discussing how they could control the population of the poor by promoting infant formula, vaccinations, sadistic hospital birthing practices, deficient government schools, and neighborhood abortion clinics. This was just too much of an assault on his strong Jewish faith and his Hippocratic oath [and why he left the club to become a medical dissident].
The Similac and Enfamil drug reps used to leave infant boy and girl growth charts at my office front desk. The charts were in stacks joined with adhesive at the top, so that you could tear off a copy and place it in the child’s chart or give it to a parent. My recollection is that before the Nestle scandal, the company’s name and logo appeared on the growth chart, but I cannot be certain of this. All the growth charts currently available are distributed by the CDC and the WHO and bear only their logos. I have no doubt that the designers of the growth charts were captured by the formula manufacturers.
Along these same lines, the public educational systems were designed so that all children were expected to develop skills like potty training, speech acquisition, ability to read, etc. in a similarly regimented growth chart fashion.* Outliers are considered “abnormal” and their parents are subjected to fear, guilt, and intimidation, and the need for the involvement of more “caring professionals”.
Also while I was practicing, when an obstetric patient was discharged from the hospital, the drug companies gave each patient a “gift bag” which included coupons for discounts and a few bottles of their formula product [and what Nestlé had gotten in trouble for doing overseas]. My hospital had one or the other of Enfamil or Similac bottles which they administered to infants if the mother allowed their baby to go to the nursery, so that the mother could “rest”, or to prevent “neonatal hypoglycemia” or “neonatal jaundice” which were other scams applied to healthy newborns designed to undermine confidence in complete breastfeeding. I am certain that the formula was provided free to the hospital, because the manufacturers knew that hospital use endorsement would generate product loyalty. When a great lactation consultant joined the nursing staff, she strongly opposed these practices, and strongly encouraged rooming-in. She would visit each mother daily to supervise and help with nursing. The established nurses did not like the lactation consultant, because they preferred to stuff the newborns with formula and wrap them tightly in warm blankets so that they would sleep and remain quiet in the nursery.
Lastly, breastmilk is digested more quickly than formula. Breast suckling is hard physical work for the baby so the baby will stop feeding when satisfied. Therefore breastfed infants wake to feed more frequently. Formula fed babies more likely to over feed because the formula flows more easily. This goes along with the weight charts issue. A seasoned pediatrician can just look at a naked baby and immediately know if it is undernourished.
Fortunately, there is now growing awareness of the predatory tactics of the formula industry (which now has an annual growth rate of 10.15% and is a 90.91 billion annual market that costs the typical parent $1,500 to $2,500 a year). For example, to quote a recent investigation by the Lancet:
For decades, the commercial milk formula (CMF) industry has used [underhanded] marketing strategies, designed to prey on parents’ fears and concerns at a vulnerable time, to turn the feeding of young children into a multibillion-dollar business. The immense economic power accrued by CMF manufacturers is deployed politically to ensure the industry is under-regulated and services supporting breastfeeding are under-resourced.
[This] three-paper Series outlines how typical infant behaviours such as crying, fussiness, and poor night-time sleep are portrayed by the CMF industry as pathological and framed as reasons to introduce formula, when in fact these behaviours are common and developmentally appropriate. However, manufacturers claim their products can alleviate discomfort or improve night-time sleep, and also infer that formula can enhance brain development and improve intelligence—all of which are unsubstantiated. Infant feeding is further commodified by cross-promotion of infant, follow-on, toddler, and growing-up milks using the same branding and numbered progression, which aims to build brand loyalty and is a blatant attempt to circumvent legislation that prohibits advertising of infant formula.
Breastfeeding has proven health benefits…however, less than 50% of babies worldwide are breastfed according to WHO recommendations, resulting in economic losses of nearly US$350 billion each year. Meanwhile, the CMF industry generates revenues of about $55 billion annually, with about $3 billion spent on marketing activities every year.
The industry’s dubious marketing practices are compounded by lobbying, often covertly via trade associations and front groups, against strengthening breastfeeding protection laws and challenging food standard regulations. In 1981, the World Health Assembly adopted the International Code of Marketing of Breast-milk Substitutes, a set of standards to prevent inappropriate marketing of formula. It includes prohibition of advertising of CMF to the public or promotion within health-care systems; banning provision of free samples to mothers, health-care workers, and health facilities; no promotion of formula within health services; and no sponsorship of health professionals or scientific meetings by the CMF industry. However, despite repeated calls for governments to incorporate the Code’s recommendations into legislation, only 32 countries have legal measures that substantially align with the Code. A further 41 countries have legislation that moderately aligns with the Code and 50 have no legal measures at all. As a result, the Code is regularly flouted without penalty.
The prioritization of trade interests over health was brought to the forefront in 2018, when US officials threatened to enforce trade sanctions and withdraw military aid to Ecuador unless it dropped a proposed resolution at the World Health Assembly to protect and promote breastfeeding. Some CMF lobby groups have cautioned against improved parental leave. Duration of paid maternity leave is correlated with breastfeeding prevalence and duration, and absence of, or inadequate, paid leave forces many mothers to return to work soon after childbirth. Lack of safe spaces for breastfeeding or expressing milk in workplaces, or facilities to store breastmilk, mean that breastfeeding is not a viable option for many women.
All information that families receive on infant feeding must be accurate and independent of industry influence to ensure informed decision making. Marketing by the CMF industry is an interconnected, multifaceted, powerful system that knowingly exploits parents’ aspirations.
Note: the complete lack of evidence for many of the medical claims on infant formulas is discussed further here.
Seed Oils In Formula
Since seed oils are linked to obesity, inflammation, and metabolic dysfunction, many parents do not want to give them to their children. In turn, I am frequently contacted by frustrated patients after they discovered that almost every infant formula is full of seed oils. After some digging, I discovered this remarkable situation (formula manufacturers refusing to sell the product customers want) was due to the following:
•FDA regulations require infant formulas to have at least 2.7% of their calories (300mg per 100 Kcal) come from linoleic acid (LA, the problematic omega-6 fat in seed oils), and the FDA aggressively enforces this. Additionally, no maximum is given, so the amount of calories from LA in formula is often much higher (e.g., 7-9% for many common brands and sometimes reaches 17%).
•This regulation arose from the Infant Formula Act of 1980 (which was virtually unanimously passed by Congress in response to more than 100 infants becoming seriously ill from nutritionally inadequate soybean oil-based formulas). Unlike most (fairly vague laws which defer to Federal agencies) this act was well-known for being extremely specific in the nutritional requirements it stipulated for infant formula.
•Those nutritional requirements were directly copied from the 1976 American Academy of Pediatrics (AAP) recommendations that did not provide an explanation for why the LA requirements were put in (which is odd given that LA was not mentioned in the AAP’s 1967 recommendations).
•The Infant Formula Act had a provision [Section 412(a)(2)] that formula nutritional requirements could be revised at any time by the Secretary of the H.H.S. Remarkably, the only changes that were ever made were raising the minimum level of calcium per 100 kilocalories from 50 to 60 mg, phosphorus from 25 to 30mg and requiring 2.0-7.0 μg of selenium (which was instituted in 2016—27 years after the Institute of Medicine determined selenium was essential for children and formula manufacturers had already begun adding it in).
So, as you might guess, nutritional science no longer supports many of the requirements in the 1980 act, but virtually all of that science has been completely ignored.
In the case of linoleic acid, (the omega-6 fatty acid), at the time the act passed, the scientific consensus was that LA was essential for infant development. This was due to data like a pivotal 1963 study of 428 infants which found infants who had less than 0.1% of their calories come from LA developed skin symptoms (e.g., drying, shedding, irritation, or infections) due to a lack of oil in the skin (along with some degree of “reduced growth”) which disappeared in those who instead received 1% of their calories from LA.
Note: another pivotal 1972 study found almost identical results when infants who had to be fed through IVs were given fat-free nutrition (where the symptoms again were interpreted as a lack of LA rather than other essential fats).
However, beyond the “necessary” amount of LA being much lower than what was subsequently required (2.7%) or what ended up in formula (e.g., the current brands I checked ranged from 7-17.1%), it also became obsolete after it was discovered that the ratio between LA to ALA (omega-3) was much more important than the LA present (e.g., too high of a LA to ALA ratio created significant issues, as did a lack of DHA). For example:
•Those early studies did not include ALA in the experimental diets, and once a bit was present (e.g., 0.5%), the need for LA was halved.
•High dietary LA has repeatedly been found to interfere with the synthesis, accumulation, and incorporation of fatty acids such as DHA.1,2,3,4,5 Likewise, decreasing the ratio of LA present was found to significantly increase DHA in tissues, particularly the brain and retina.1,2
Note: DHA is essential for brain and eye development, but unfortunately like ARA, it is quite fragile and easily damaged during the manufacturing process (whereas in homemade formulas and human breastmilk they are not).
•One reason LA was considered “essential” is because the body converts it to arachidonic acid (ARA), which is critical for brain and nervous system development. However, in infants, the conversion is very poor (estimates range from 0.2-5%—this study for instance found infants only converted 1.2% of ingested LA to ARA), so infants require ARA rather than its LA precursor (e.g., 0.55% of the fats in human breastmilk are ARA).
Note: the levels of ARA and DHA are heavily dependent on the mother’s diet (e.g., one study found a Chinese community which consumed a traditional post-labor diet quite high in eggs, poultry and pork had significantly higher levels of DHA, ARA, and total fat content in their breastmilk, while when those mothers switched to consuming seed oils, harmful fats increased in their breastmilk). Likewise, the presence of choline (another critical nutrient for many developing tissues, including the brain) in breastmilk highly depends on the mother’s diet (e.g., eggs and liver being excellent dietary sources).
•High dietary LA does not support the growth of developing neurons, and in humans, it has been linked to atypical neurodevelopment and impaired motor and cognitive scores early in life.
•High dietary LA increases the brain’s vulnerability to inflammation.
In short, a strong case can be made that much of the original data arguing for the necessity of LA in formulas actually due to a lack of other essential fats, but rather than heed this, we opted to use an incredibly excessive amount of LA while simultaneously ignoring all of the science from the last 50 years that demonstrated the other fats needed to be focused on (and that, as a 2016 systematic review showed, we still have very poor data for these nutritional guidelines). Most remarkably, while other regulators (e.g., in China and Europe) have required fats like DHA to be included and lower LA to ALA ratios, the FDA has not (but will target companies who do not stuff their formulas with seed oils).
Note: while the government will often be extremely stubborn and refuse to correct a longstanding mistake (perfectly demonstrated by this example), I strongly suspect the unwillingness to fix the linoleic acid requirements was significantly influenced by lobbying (as LA is one of the cheapest ingredients available to the processed food industry). Likewise, many believe the medical literature is so hostile to home formula options because industry money was spent to eliminate any potential competition.